Product Updates
Automated Claim-Line Repricing
For years, network benchmarking has been… kind of a mess. Carrier repricing is free, sure — but it’s subjective, inconsistent and opaque. UDS is based on years-old claims and takes time to turn around.
We knew we could do better. So we did.
We built automated claims repricing directly into Iris.

Upload your claims file, and in minutes you’ll get:
Repricing across both hospital and carrier rates
Outputs in dollars and Medicare percentages
Reports you can actually use with clients
No more guessing. No more waiting. And no more relying on stale data that doesn’t hold up under scrutiny.
We designed this to make the truth easy to access — and impossible to ignore.
In the News
Pricing Data Impacts To Plans
Our Takeaway: Employers are becoming increasingly vocal about understanding detailed pricing data by procedure, geography and provider. Brokers and TPAs will need to provide deeper insights and strategies than before to prove their recommended approach is the best option.
Our Takeaway: Employers are getting savvy about the price-value equation, and with price transparency data are negotiating higher quality care within their plans.
Data Insights
Aetna PPO Rate Changes
What we’re seeing (Q3 refresh):
Fewer fee-for-service (FFS) rates in Aetna’s source data
More contracts priced as a %-of-billed rather than fixed FFS
Inpatient: providers on %-of-billed rose from 12% to 48% (April → July 2025, depicted below)
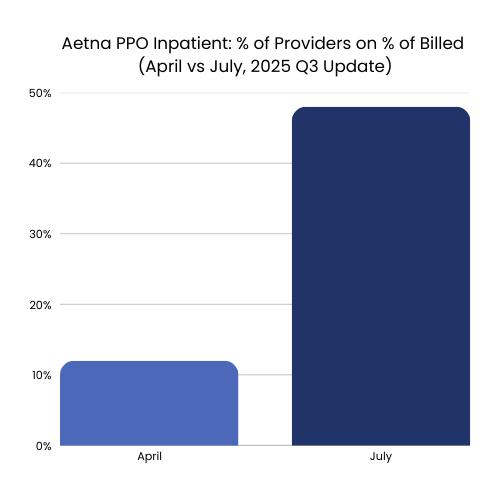
Why it matters:
Signals a contract shift: The move from fixed FFS to %-of-billed points to real contractual changes and may indicate a broader macro trend in the pricing models providers are willing to use.
We’re refreshing Aetna’s files in September 2025 and will share any new or notable changes as soon as they’re live.
From the Desk of Ahmed
What’s Top of Mind for the Brokers I’m Speaking With…

Ahmed Marmoush, CEO & Co-Founder, Handl Health
Hi, Ahmed here!
I’ve had the chance to speak to a number of brokers over the past month about the questions they’ve been getting from their prospects and clients over the course of renewal season.
Doubling down on data: Brokers are leaning into analytics to differentiate themselves, showing employers not just renewal options but real performance comparisons between networks and carriers. This shift is reshaping how employers evaluate their advisors—data has become the new table stakes.
Execution is the biggest question: While brokers are presenting smart, forward-looking strategies, many struggle to deliver on the operational side—whether that’s managing direct contracts, implementing transparency tools or driving member engagement. The so what: employers are starting to ask not only “who has the best ideas?” but “who can actually make them real?”
Evaluating effectiveness within the plan year: Employers no longer want to wait until renewal season to understand if a plan is working. Brokers are being pushed to provide in-year insights on spend, utilization and outcomes—helping clients identify and act on cost drivers before they become end-of-year surprises.
Recap
That’s all for the first issue of Re:Pricing. Thanks for being part of our community that values clarity over complexity in healthcare pricing.
If you have feedback or topics you’d like us to cover in future editions, just hit reply — we’d love to hear from you.
— The Handl Health Team



