Product Updates
Disruption, Made Simple
When we launched our Network Evaluation template, it opened up a new level of transparency for brokers and consultants, finally giving them the tools to compare rates, assess coverage and identify misaligned providers.
But some decisions demand even more precision.
That’s why we built the Disruption template: a purpose-built tool to help you model network changes with confidence.
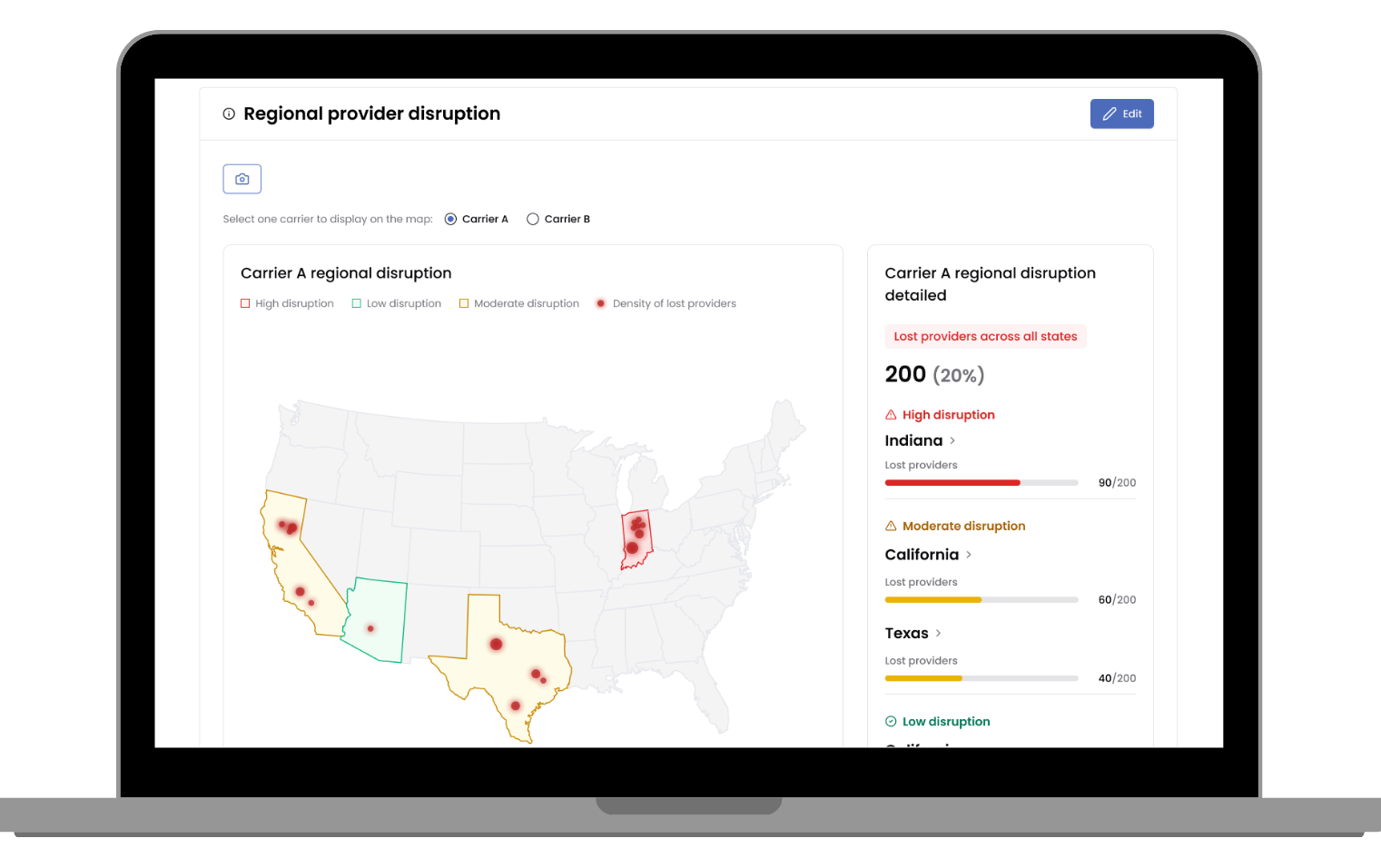
With the Disruption template, you can:
Compare provider inclusion across networks
Identify which NPIs are exclusive, overlapping or missing
Quantify disruption at the provider and claim level
It builds on what we started...and takes it even further.
Because smart network design isn’t just about understanding what you have. It’s about knowing what’s possible.
In the News
Hospital Price Transparency Is Working
Our Takeaway: Valuable hospital pricing data being public doesn’t immediately translate into consumer benefit without friendly tools to access the data. Expect more consumer-oriented pricing tools to hit the market and create upward pressure on hospitals to release more detailed data.
Improving Prescription Drug Price Transparency
Our Takeaway: With the introduction of the drug price transparency tool, we will continue to move closer to enabling consumers to easily shop for prescriptions based on the patient-specific cost, forcing pharmacies to compete and providing price pressure on PBMs and drug companies.
Data Insights
ASC vs. Hospital Rates
What we’re seeing:
It’s no surprise that ambulatory surgery centers (ASCs) are typically less expensive than hospitals. But now, we can see exactly how much cheaper.
In the Boston, MA area, hospital rates are on average ~125% higher than ASCs. For example, CPT 24358 (tendon repair in the upper arm/elbow) is priced significantly higher at hospitals ($5,575) compared to ASCs ($2,535) — shown below.
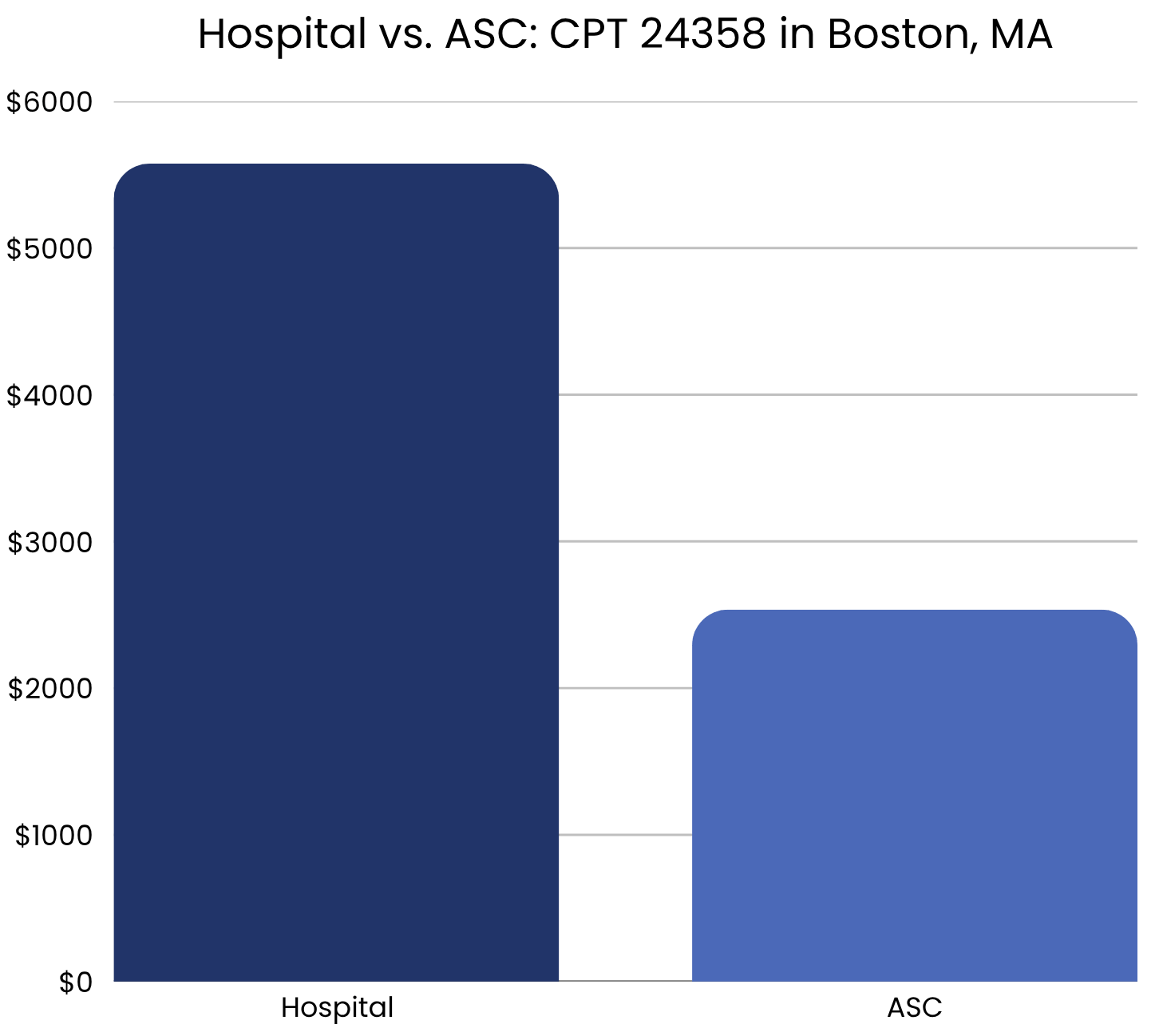
Why it matters:
Understanding how much more expensive hospitals are changes the conversation. Everyone knows there’s a gap—but quantifying it allows brokers, consultants and employers to:
Design smarter plans: Without site-of-care steerage built into plan design, members default to the most expensive setting.
Empower member decisions: When employees have visibility into true cost differences, they’re more likely to choose a lower-cost, high-quality ASC.
Leverage data for negotiations: Exact rate comparisons strengthen employers’ ability to hold carriers and providers accountable.
The takeaway:
Site-of-care differentials are one of the most consistent, predictable drivers of excess healthcare spend. While the fact that ASCs are cheaper isn’t new, having clear, local, CPT-level rate data makes it actionable. With the right plan design, decision-support tools and access to transparent data, employers can move members toward value—lowering claims costs, protecting employees from unnecessary bills and reinforcing fiduciary responsibility.
From the Desk of Ria
Top 3 Data Questions From Brokers…

Ria Shah, Chief Product Officer & Co-Founder, Handl Health
Hi, Ria here!
When questions come in about the pricing data in our tools, I’m always happy to talk to brokers about their top concerns.
Here’s what I’m hearing from recent conversations…
How reliable are the hospital & carrier transparency files—can I use them with confidence?
Short answer: yes, with guardrails. File quality varies by publisher, so we run validation to catch missing rates, weird outliers, and duplicates, then label each record with a confidence score. Treat the data like a powerful flashlight—use it to illuminate patterns and directional comparisons, and pair it with context when you make recommendations.
Why do I sometimes see two different rates for the same provider and service—and which one is “right”?
Duplicate rates happen (think DRG A at $23k vs. $29k in the same file). We resolve that by ranking records with a confidence score informed by benchmarks (e.g. Medicare-relative reasonableness and historical commercial claims). When rates are close and both look plausible, we select the higher-confidence record and flag the rest—so you can proceed without getting stuck in the weeds.
How “complete” is the data, and what happens when there are gaps?
Coverage can be uneven by market or plan. We routinely hit high code coverage in many MSAs, but when a slice is missing or clearly low-quality, we won’t force it—there’s a floor. In those cases we use derived (synthetic) rates at the clinical-category level, anchored to validated patterns we do see. The goal is practical usability: keep reports decision-ready while avoiding false precision. Let me know if you’re curious about our methodology for deriving missing rates, I’d be happy to walk you through it.
What questions do you have about the price transparency data? Reach out and ask!
Are you going to SIIA in Phoenix?
Ahmed and Shapari will be there and would love to say hello! Book a time slot and we’ll come to you.